20 March 2026
Mandy Melissa Jane Wittens
As healthcare systems are increasingly data-driven, combining data from different sources is becoming essential to improve care, reduce inefficiencies, and support better decision-making. While clinical data is routinely collected, important information about patients’ daily nutrition often remains invisible in digital health systems. The staff may know which meals are served but have limited insight into how much food patients actually consume. As a result, early signals of malnutrition, poor appetite, or systematic food waste may remain unnoticed. Yet nutrition plays a crucial role in patient recovery, wellbeing, and long-term health outcomes, particularly for elderly or vulnerable populations.
Improving the collection and use of food intake data offers a dual opportunity: to strengthen healthcare quality and to operate institutional food services more sustainably. By capturing what patients actually eat and linking this information to other health and nutrition datasets, care providers and researchers can support better monitoring, personalised nutrition strategies, and operational efficiency.
The FINE (Food Intake Ecosystem) project explores how personal food intake data can be captured and integrated into broader health data infrastructures to reduce food waste in care settings. Through stakeholder workshops involving actors from healthcare, food services, technology, and research, the project investigated how such data could be shared and combined within a Food & Health Data Space
Highlights
| Food intake data is largely missing from healthcare systems, creating a blind spot in detecting malnutrition and reducing food waste |
| Integrating food intake and health data can improve patient care by uncovering patterns, enabling personalisation, and informing preventive strategies |
| A Food & Health Data Space can strengthen cross-sector collaboration, connecting healthcare providers, food suppliers, researchers, and technology companies. |
| Trust, governance, and interoperability are key barriers: unclear ownership, privacy concerns, incompatible systems, and governance uncertainties must be addressed. |
1. Why food intake data matters
A half-eaten plate can tell a whole story. It may signal declining health, poor appetite, or meals misaligned with patients’ preferences. Left unnoticed, these gaps can result in lost nutrition, wasted resources, and avoidable environmental impacts. Studies estimate that up to 30–40% of hospital and care centre meals go uneaten, often due to patient preferences, dietary restrictions, or portion sizes. Systematically capturing food intake allows care providers to monitor nutritional status, tailor meals, reduce waste, and evaluate the effectiveness of nutrition policies. For elderly and vulnerable patients, accurate intake data supports recovery, wellbeing, and long-term health, while helping institutional food services operate more sustainably and efficiently.
1.1. What is FINE?
The FINE (Food Intake Ecosystem) project, which is supported by VLAIO and carried out in collaboration with Biovia, Flanders’ Food, imec, ILVO, and VIVES, explores how accurate data capture of personal food intake can contribute to these goals. Using an existing measurement setup that can quantify the amount of food served and the amount remaining on the plate, the project demonstrates how detailed food intake data can be captured in real-life care settings. Data alone, however, is not enough. To generate meaningful insights, food intake data must be combined with other relevant datasets, such as nutritional information, patient health data, and operational data from kitchen and care systems. This requires multiple actors, often working in separate domains. To explore how such data could be shared and combined, FINE organised a series of stakeholder workshops. These sessions aimed to build knowledge about data spaces and identify the practical requirements, opportunities, and challenges for cross-organisational data sharing.
1.2. Food and health data in the European landscape
A Food & Health Data Space aligns with broader European initiatives for trusted cross-sector data sharing. The European Health Data Space (EHDS) enables secure access, exchange, and secondary use of health data, while promoting transparency, interoperability, and responsible data governance. Similarly, the Common European Agricultural Data Space aims to improve transparency, sustainability and data-driven innovation in the agri-food sector. Food intake data sits at the intersection of these domains. When linked with clinical and nutritional information, it can illuminate relationships between diet, health outcomes, and food system efficiency. A Food & Health Data Space could therefore complement existing European initiatives, connecting healthcare, food services, research, and technology while operating under GDPR, the Data Governance Act, and the Data Act.
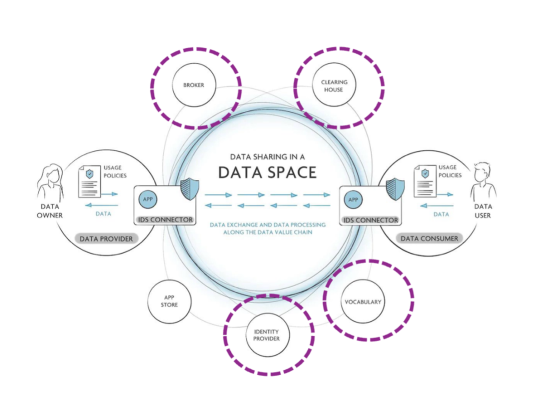
Image 1: Data space overview
2. Data space requirements workshop
2.1. Understanding the roles in a data space
To make the concept of a data space more tangible, the workshops introduced several key roles that help organise how data can be shared between different actors. For example:
- A Broker is a service that enables the publication and discovery of data resources and services within the data space. Data providers can register their datasets, and data consumers can search for relevant data offerings through this catalogue function.
- A Clearing House provides logging and accounting services for data transactions. It records when and under which conditions data exchanges occur, enabling traceability, compliance with usage policies, and potential billing or auditing of data usage.
- An Identity Provider is responsible for authentication and identity management within the data space. It verifies the identity of organisations and users that want to participate, ensuring that only trusted and authorised participants can access data and services.
- A Vocabulary Provider maintains shared semantic models, ontologies, and vocabularies that define how data should be described. By providing common definitions and metadata standards, it ensures that data coming from different systems can be understood, combined, and interpreted consistently across participants.
By exploring these roles through scenarios and roleplay exercises, participants gained a better understanding of how a data space can enable secure and structured data sharing while allowing organisations to retain control over their own data.
2.2. Data sharing reflections
The workshop discussions provided valuable insights into how stakeholders perceive the potential of a Food and Health Data Space. Several opportunities and barriers were identified.
2.2.1. Opportunities
Participants highlighted that by linking food intake data with patient health records, nutritional information, and operational data, organisations could detect patterns that are otherwise invisible, such as which meals are consistently uneaten, how nutrition correlates with recovery outcomes, or where food waste is highest. Combined datasets could also improve decision-making and service planning. For example, dietitians could adjust meal options based on actual consumption patterns, kitchen managers could optimise portion sizes to reduce waste, and policymakers could identify systemic gaps in nutrition support across care institutions. Cross-actor data sharing also reduces duplication of effort, allowing each organisation to focus on its expertise while still benefiting from insights gathered elsewhere. Ultimately, this supports personalised care tailored to individual patients’ needs.
2.3. Barriers
Despite the potential benefits, participants highlighted several challenges that currently limit data sharing. Interoperability was a major concern: food service systems, electronic health records, and kitchen management tools often use different formats and definitions, making it difficult to link food intake data with health and operational datasets. Data ownership and responsibility were also unclear. Stakeholders questioned whether the patient, the care organisation, or technology providers hold the rights to food intake data, creating hesitation to share information. Privacy and data protection were equally critical, since linking food consumption with health data involves sensitive personal information that must comply with GDPR and other regulations. Finally, competition can act as a barrier. Technology providers or food suppliers may be reluctant to share data if they fear losing commercial advantage or revealing proprietary insights.
3. Requirements for a Food & Health Data Space
The workshop identified several key requirements for a functioning Food & Health Data Space.
1) Transparency and traceability are essential: data providers must see who accessed their data, when, and for what purpose, supported by logging and audit mechanisms.
2) Control over data use is equally important. Data owners should be able to explicitly approve access through opt-in mechanisms, specify conditions for how their data may be used, such as research vs. commercial purposes, and withdraw consent through opt-out mechanisms. Patients should also be able to access high-level information on how their data is used.
3) Safeguards are needed for exceptional situations, such as public health crises, where government authorities may use aggregated data, and, where necessary, override the data owner, when this is essential for the public interest or public health. This follows a “glass-break” principle and should operate under clear governance rules.
4) Data quality and shared responsibility were also critical, with all actors, providers, intermediaries, and users, have a shared responsibility to ensure minimum standards, accurate metadata, and mechanisms to correct errors or address repeated violations.
5) The ecosystem must be organisationally and financially sustainable, with models such as membership fees, transaction charges, or cooperative funding structures to cover onboarding, system maintenance, and governance. It should also address the common imbalance where data providers bear most of the costs (collection, cleaning, standardisation) while many benefits accrue to data users, by ensuring fair compensation or other incentives for providers.
Realising these requirements depends on cross-sector collaboration. Healthcare organisations, food suppliers, kitchen services, technology providers, and researchers must align on standards, governance, and rules for data sharing. Stakeholders are generally open to sharing, but only under clear conditions of trust, transparency, and control, addressing concerns around data ownership, privacy, interoperability, and competitive advantage. The FINE project represents an important first step, combining practical experimentation with stakeholder engagement to identify the opportunities, barriers, and requirements that will guide future developments in a Food & Health Data Space.
| Develop shared standards for food intake and nutrition data |
| Efforts supporting the development of common data standards and shared vocabularies for food intake, nutritional information, and related health data are essential, to ensure that datasets from different origins can be combined and interpreted consistently. |
| Establish clear governance frameworks for data sharing |
| The development of a Food & Health Data Space requires transparent governance structures that define roles, responsibilities, and decision-making processes. Policymakers should support governance models that clarify how data can be accessed, shared, and monitored while ensuring accountability among participating actors. |
| Ensure strong privacy protection and data control mechanisms |
| Trust is a key condition for data sharing. Data owners, including care organisations and patients, must retain control over how their data is used, supported by mechanisms such as opt-in consent, clear usage policies, and transparent logging of data access. |
| Stimulate cross-sector collaboration between healthcare and food systems |
| Building a Food & Health Data Space requires collaboration between actors that traditionally operate in separate domains. Policymakers and sector organisations should encourage partnerships between healthcare providers, food companies, technology developers, and research institutions. |
| Invest in data maturity and data literacy within care institutions |
| Many organisations still face challenges related to data management capacity and data literacy. Supporting stakeholders in developing these skills is essential to enable effective data sharing and ensure that data can be used responsibly and effectively. |
DOWNLOAD THE POLICY BRIEF
About the author
Mandy Melissa Jane Wittens is a postdoctoral researcher in the EDDI (Ethics by coDesign in Digital Innovation) at imec-SMIT, VUB, focusing on the secondary use of healthcare data, data spaces, and how insights from data can support decision-making, improve care delivery, and strengthen patient outcomes.
About the Ethics by coDesign in Digital Innovation (EDDI) unit
EDDI is a research unit at imec-SMIT, VUB that develops participatory, human-centred methods to embed ethics, transparency, and societal values in digital and AI innovations, with a focus on healthcare, work, and public services. It combines academic research with practical guidance through the Knowledge Centre Data & Society and is led by prof. An Jacobs and prof. Rob Heyman
See more information about the FINE project at:
- https://www.flandersfood.com/nl/nieuws-new-flanders-food/2022/food-intake-ecosystem-fine
- https://www.flandersfood.com/nl/projecten/fine-food-intake-ecosystem
Project partners


